Endothelial dysfunction might lead to vasoconstriction. NO activates guanylate cyclase which
Know the therapeutic goals for treating angina.
See also Brody p 240 – table citing "therapeutic overview"
Coronary artery insufficiency – increase effective flow through the coronary
arteries and ¯ O2 consumption by the
heart. Goal is also to prevent vasospasm of coronary arteries.
Know the cardiovascular effects of nitric oxide (NO) and how endothelial
dysfunction might lead to vasoconstriction.
Endothelial dysfunction might lead to vasoconstriction. NO activates
guanylate cyclase which ![]() cGMP which leads to
dephosphorylation of myosin-light-chain-kinase (MLCK). Effects on the CV system:
cGMP which leads to
dephosphorylation of myosin-light-chain-kinase (MLCK). Effects on the CV system:
Note: Brody, p 240 comments on "steal" phenomenon: The ischemic are of heart is already vasodilated due to the metabolic end products; vasodilation by drugs does "little to enhance blood flow to ischemic region."
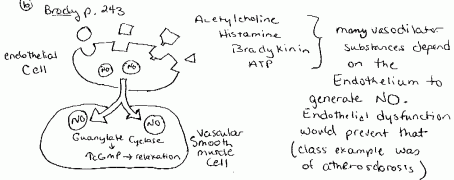
Acetylcholine, histamine, bradykinin, ATP – many vasodilator substances depend on the endothelium to generate nitric oxide. Endothelial dysfunction would prevent that (class example was atherosclerosis).
Understand the mechanisms of action of nitrates and Ca+2 channel
blockers, and relate them to the rationale for using these drugs for treating
angina.
NO activates guanylate cyclase which ![]() cGMP
which leads to dephosphorylation of myosin-light-chain-kinase (MLCK). Effects on
the CV system:
cGMP
which leads to dephosphorylation of myosin-light-chain-kinase (MLCK). Effects on
the CV system:
Angina is O2 demand > supply.
Nitrates ¯ demand, also
vasodilate the coronary arteries but the "steal phenomenon means ischemic
tissue doesn’t necessarily benefit. Nitrates also ![]() supply.
supply.
Ca+2 channel blockers ¯
demand by ¯ afterload of arterial beds and ![]() supply.
supply.
Discuss the rationale of co-administering b
-blockers with vasodilators, in the treatment of angina.
Vasodilators can cause reflex tachycardia via SNS
stimulation. b -blockers inhibit the ![]() HR (which would have
HR (which would have ![]() ed O2 demand and
worsened angina.
ed O2 demand and
worsened angina.
Be able to distinguish the vascular and cardiac effects of the 3 classes of Ca+2 channel blockers.
|
Phenylalkylamine |
Dihydropyridines |
Benzothiazepine |
|
|
Vasodilation |
|||
|
Peripheral |
++ |
+++ |
+ |
|
Coronary |
++ |
+++ |
+++ |
|
Cerebral |
+ |
+ |
+ |
|
Heart rate |
¯ |
|
¯ |
|
SA node |
¯ |
¯ ¯ |
|
|
AV node |
¯ ¯ |
¯ |
|
|
Contractility |
¯ ¯ |
|
¯ |
| Indications For Use |
Prinzmetal’s angina, Chronic stable angina, PSVT, Afib/flutter, essential HTN |
Angina caused by spasm, chronic stable angina, HTN |
Prinzmetal’s angina, chronic stable angina, HTN |
| Notes |
Open channel blocker so channel must be open to work. |
Called L-type channel blockers. Prefers channel closed & more negative. |
|
Know the pharmocokinetics (routes of administration, relative time of absorption, onset and duration) of each class of antianginal drug.
Know the clinical problems for each class (especially related to the mechanisms of action).
Nitrates:
b -blockers:
Ca+2 channel blockers:
Last updated 09/06/01 08:53 PM
Return To The MNA 2001 Homepage